by Ken Sehested
Last fall one of our local journalists, who has an “answer man” column devoted to readers’ questions, was asked about hospitalization insurance coverage, particularly why some of the services received were covered by  insurance but others (the ones in small print about “out-of-network” exceptions) were not.
insurance but others (the ones in small print about “out-of-network” exceptions) were not.
The hospital president wrote an explanation. This was my response.
Kudos for John Boyle’s “answer man” column, “Answer Man: Does Mission have ‘out-of-network’ staff docs?”, devoted to the labyrinthine health care coverage puzzle, particularly the out-of-network rules which few but the lawyered-up can solve, though Mission Hospital CEO Dr. Ron Paulus did his best to (in the words of George Orwell) “give the appearance of solidity to sheer wind.”
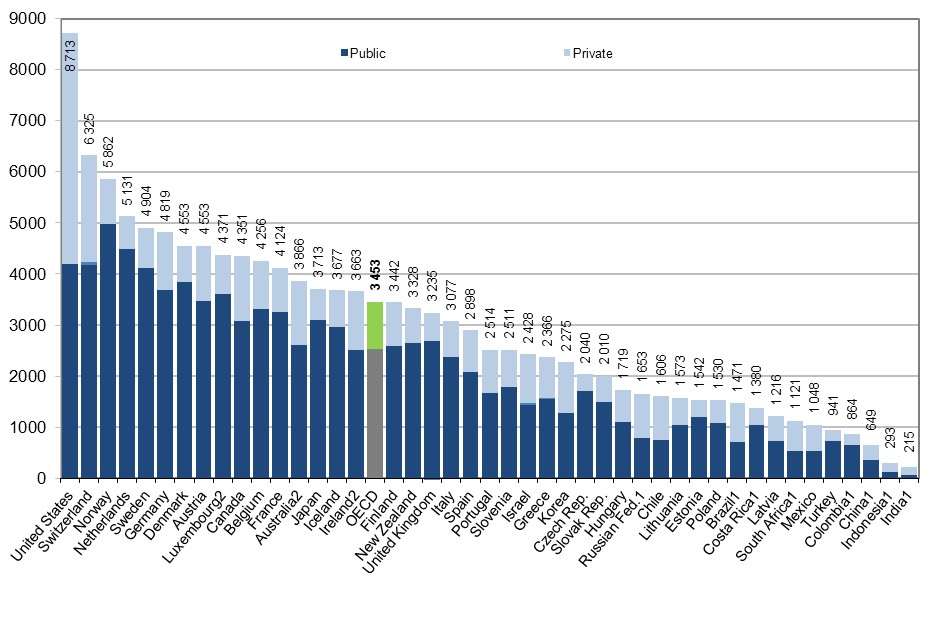
Unfortunately, this is a case where conclusions failed to factor in overlooked premises: The complexity is not in the nature of things but is orchestrated by unexamined values, resulting in the fact that Americans spend more health than any other developed nation but are among the least healthy.
One place we excel is administrative job security: For every three doctors in the U.S. there are two staffers handling paperwork. [1]
To adequately explore more productive options requires attention to at least three factors often left out of the conversation.
1. Some basic level of health care ought to be considered a fundamental human right, along with free speech, the right to vote, and all other recognized provisions for what it means to pursue “life, liberty, and the pursuit of happiness.” When our Constitution was written, “happiness” was not a subjective emotional state but an objective condition of well being.
The U.S. is the only industrialized country in the world that lacks universal health care. We won’t get there until our nation’s commitment to “the common defense” and “general welfare” provisions of The Declaration of Independence include health care as an “inalienable right.”
2. Removing profit motives as the engine of health care delivery is essential. For an example of how “market” values have come completely unhinged with regard to human well-being, ponder this statement from J. Michael Pearson, CEO of Valeant Pharmaceuticals, on the practice of buying up drug patents and jacking the price—56 such drugs raised an average of 66% in 2016:
“My primary responsibility is to Valeant shareholders. We can do anything we want to do. We will continue to make acquisitions, we will continue to move forward.” [2]
“Socialized” medical care—a single-payer system—should be no more frightening that socialized traffic laws, policing, fire fighting, and public education.
Sure, there is plenty of room for debate what constitutes a basic level of health care that should be guaranteed. But we engage in such debates, and make decisions (many of which change over time), on a regular basis. We can do this.
3. The existing medical care culture, in all its institutional forms, needs to shift from a “sick” care to a “health” care model. Needed wisdom is no more complex than the well-worn aphorism, “a stitch in time saves nine.”
The root of the problem is that “economic and technological factors dating from the early 20th century remain strong barriers to effective disease prevention. A key feature of U.S. health care is its use of a piecemeal, task-based system that reimburses for ‘sick visits’ aimed at addressing acute conditions or acute exacerbations of chronic conditions.” [3]
The levels of complexity in health care will only increase until these assumptions are examined and overturned.
# # #
[1] Sarah Kliff, “8 facts that explain what’s wrong with American health care,” Vox
[2] “ Valeant CEO J. Michael Pearson Speaks One-on-One with Meg Tirrell Today on CNBC,” 28 May 2014
[3] Farshad Fani Marvasti and Randall St. Stafford, “From Sick Care to Health Care—Reengineering Prevention into the U.S. System,” The New England Journal of Medicine, 6 September 2012

